Tooth pain during pregnancy affects more than half of expectant mothers, yet it’s often dismissed as a minor inconvenience. In reality, hormonal surges, increased blood flow, morning sickness, and intense food cravings create a perfect storm for gum disease, enamel erosion, and tooth decay. Left unmanaged, dental pain isn’t just uncomfortable—it can increase the risk of serious complications like preterm birth and low birth weight. The good news? Most dental treatments and pain relief methods are safe during pregnancy. This guide delivers practical, expert-backed strategies to relieve tooth pain safely, covering home remedies, medication safety, professional care by trimester, and prevention—all tailored to protect both you and your baby.
Why Pregnancy Increases Your Risk of Tooth Pain
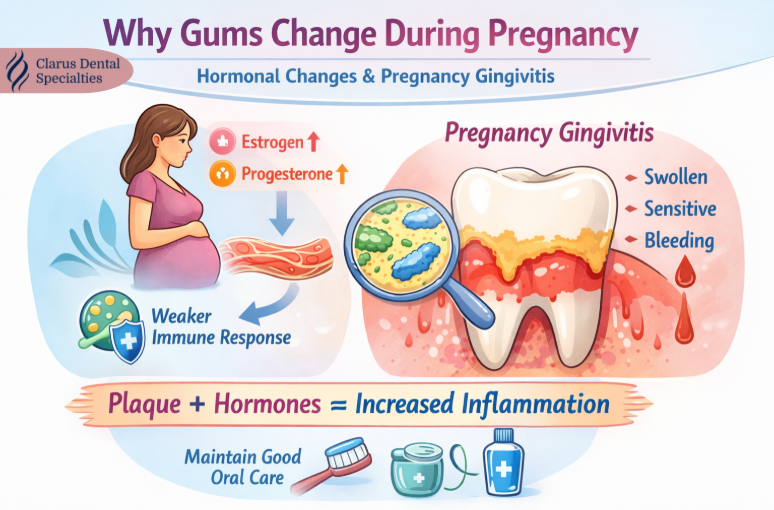
Pregnancy changes your body in ways that directly impact oral health. Recognizing these triggers helps you respond before minor discomfort turns into a serious problem.
Hormonal Surges Trigger Gum Inflammation
Rising progesterone and estrogen levels increase blood flow to your gums, making them more reactive to plaque—even if you brush and floss regularly. This can lead to pregnancy gingivitis, which affects up to 75% of pregnant women. Symptoms include red, puffy gums that bleed when brushing, increased tooth sensitivity, and pain around the gum line. Left untreated, this inflammation can progress to periodontal disease, which has been linked to adverse pregnancy outcomes.
Stomach Acid Erodes Enamel After Vomiting
Morning sickness isn’t just hard on your stomach—it’s damaging to your teeth. Stomach acid softens enamel within seconds of vomiting. Brushing too soon afterward can wear it down faster, leading to sensitivity, cavities, and erosion. Rinsing with a baking soda solution (1 tsp in a glass of water) neutralizes acid safely without harming enamel.
Sugar Cravings Feed Cavity-Causing Bacteria
Pregnancy cravings often lean toward sweets and carbs, which feed harmful oral bacteria like Streptococcus mutans. Frequent snacking without brushing increases plaque buildup and acid attacks on teeth. If nausea makes oral hygiene difficult, the risk of decay rises significantly.
Pregnancy Tumors Can Cause Discomfort
Also known as pyogenic granulomas, these benign red or purple growths appear on the gums, usually in the second trimester. Though not dangerous, they bleed easily and can make eating or brushing painful. Most resolve after delivery, but they may require monitoring or minor removal if they interfere with daily life.
Immediate Home Remedies That Actually Work

While home remedies won’t cure infections or cavities, they can provide safe, temporary relief from tooth pain during pregnancy.
Saltwater Rinse to Reduce Swelling and Kill Bacteria
Mix ½ to 1 teaspoon of salt in a cup of warm water. Swish for 30 seconds, then spit—do not swallow. This simple rinse reduces inflammation by drawing fluid out of swollen gums, kills bacteria, and balances oral pH. Use 2–3 times daily, especially after meals or vomiting.
Cold Compress for Facial Swelling and Nerve Pain
Wrap an ice pack or frozen peas in a soft cloth and apply to the outside of your cheek for 15–20 minutes. The cold constricts blood vessels, reducing swelling and numbing nerve pain. Avoid direct skin contact to prevent frostbite.
Clove Oil for Fast, Natural Numbing
Dilute 1 drop of clove oil in 1 teaspoon of coconut or olive oil. Apply gently to the painful tooth with a cotton swab. Eugenol, the active ingredient, acts as a natural anesthetic and antiseptic. Avoid swallowing and do not use on open sores. Consult your OB-GYN before using in the first trimester.
Baking Soda Paste to Neutralize Acid and Soothe Gums
Mix baking soda with water to form a paste. Apply directly to sensitive areas or use as a rinse. It neutralizes acid, reduces bacteria, and calms irritated tissues. Safe if small amounts are accidentally swallowed.
Garlic for Antibacterial Relief
Crush a fresh garlic clove and place it on the affected tooth. Allicin, a compound in garlic, fights bacteria and may help prevent infection. It’s effective but can cause temporary bad breath.
Herbal Rinses (Peppermint, Chamomile) for Calming Relief
Brew a cup of peppermint or chamomile tea, let it cool, and swish for 30 seconds. Menthol soothes nerves, while chamomile reduces inflammation. Never use concentrated herbal extracts—stick to mild tea and check with your doctor first.
Aloe Vera Gel to Heal Inflamed Gums
Apply purified, oral-safe aloe vera gel directly to swollen or bleeding gums. Its anti-inflammatory compounds promote healing. Avoid products containing aloe latex, which can be unsafe during pregnancy.
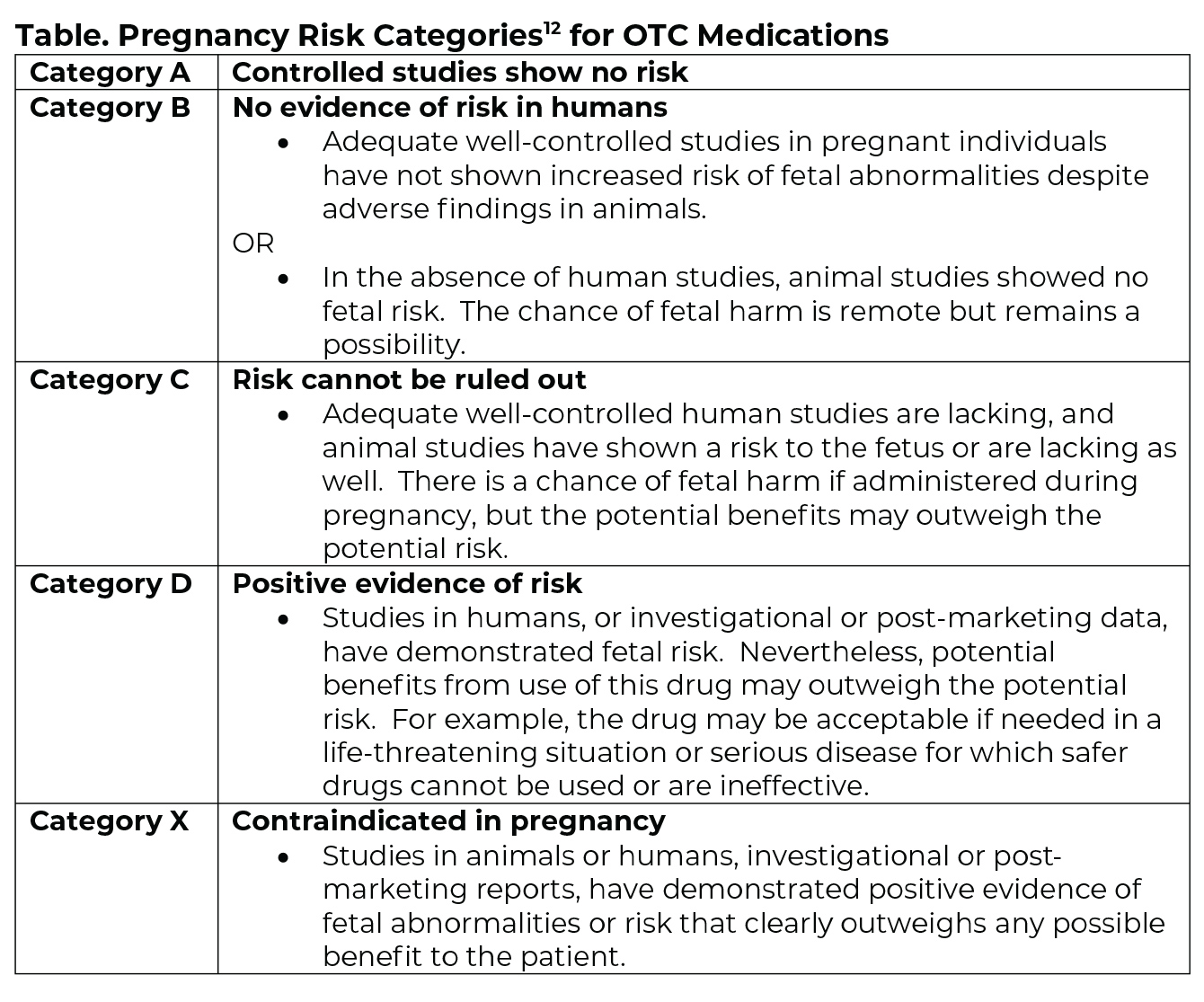
What Painkillers Are Safe During Pregnancy?
When home remedies aren’t enough, medication may be necessary—but not all options are safe.
Acetaminophen (Tylenol) Is the Only Recommended OTC Option
For mild to moderate tooth pain, acetaminophen is considered safe in all trimesters when used as directed. Typical dosage is 500–1000 mg every 4–6 hours, not exceeding 3000–4000 mg per day. Always confirm with your OB-GYN, especially if you have liver issues or other health conditions.
Avoid Ibuprofen, Aspirin, and NSAIDs
- Ibuprofen (Advil, Motrin): Not safe in the third trimester—linked to reduced amniotic fluid and heart complications in the baby.
- Aspirin and naproxen (Aleve): Increase bleeding risk and are not recommended unless prescribed.
- NSAIDs in general: Avoid unless explicitly approved by your doctor.
Use Topical Gels with Caution
Benzocaine gels (like Orajel) can numb pain temporarily but should be used sparingly. Overuse may cause rare but serious side effects like methemoglobinemia. Avoid alcohol-based products, which can dry and irritate sensitive tissues.
Safe Dental Treatments by Trimester
Dental care is not only safe during pregnancy—it’s essential. Infections can spread and harm both you and your baby.
Second Trimester: Ideal for Non-Emergency Dental Work
Weeks 13 to 27 are the safest window for fillings, cleanings, root canals, and other non-emergency procedures. Nausea often improves, and the baby’s major organs have already developed. This is the best time to address cavities or gum disease.
First Trimester: Limit to Emergency Care Only
Avoid elective procedures. Focus on pain relief, infection control, and hygiene. If urgent care is needed, local anesthesia (like lidocaine) is safe when used appropriately.
Third Trimester: Short, Necessary Visits Only
Lying flat for long periods can reduce blood flow to the baby. Dentists can tilt the chair or use pillows for comfort. Postpone non-urgent treatments until after delivery.
Approved Dental Procedures and Medications
Know what’s safe so you can advocate for your care without fear.
Fillings, Cleanings, and Root Canals Are Safe
Amalgam and composite fillings, professional cleanings, and root canals can all be performed during pregnancy. Treating infections promptly protects your health and your baby’s.
X-Rays Are Safe with Protection
Dental X-rays use extremely low radiation. With a lead apron and thyroid collar, the risk is negligible. X-rays are often necessary to diagnose abscesses or hidden decay.
Safe Antibiotics Include Penicillin and Amoxicillin
If an infection is present, your dentist may prescribe:
– Penicillin
– Amoxicillin
– Erythromycin
Avoid tetracycline and doxycycline—they can stain your baby’s developing teeth.
Anesthesia and Sedation Are Generally Safe
- Lidocaine: Safe in all trimesters at the lowest effective dose.
- Nitrous oxide (laughing gas): Low-dose use is acceptable—discuss with your OB-GYN.
- General anesthesia: Reserved for emergencies and requires coordination with your OB team.
Prevent Tooth Pain Before It Starts
The best way to avoid pain is to prevent it.
Stick to a Daily Oral Hygiene Routine
- Brush twice daily with a soft-bristled brush and fluoride toothpaste.
- Floss every day—most cavities start between teeth.
- Use an alcohol-free mouthwash to avoid dryness.
- Try a water flosser if traditional flossing irritates your gums.
Eat a Tooth-Protective Diet
- Calcium: Yogurt, milk, kale, almonds—supports your teeth and baby’s bones.
- Vitamin D: Fatty fish, eggs—helps absorb calcium.
- Vitamin C: Strawberries, oranges, bell peppers—strengthens gums.
- Hydrate with water: Rinses away food and bacteria.
Care for Teeth After Vomiting
Wait 30 minutes before brushing. Rinse with water or a baking soda solution instead. Chew sugar-free xylitol gum to stimulate saliva and neutralize acid.
Don’t Share Utensils or Food
Cavity-causing bacteria can be passed to your baby through saliva. Avoid sharing spoons, cups, or testing bottle temperature with your mouth.
When to See a Dentist Immediately
Don’t wait if you have:
– Severe, throbbing pain
– Facial, jaw, or neck swelling
– Fever or chills
– Pus or a bad taste in your mouth
– Trouble swallowing or breathing
These signs may indicate a dental abscess—an infection that requires urgent treatment. Untreated, it can lead to preterm labor, low birth weight, or even maternal sepsis.
Coordinate Care Between Your Dentist and OB-GYN
Your safety depends on teamwork:
– Tell your dentist you’re pregnant and your current trimester.
– Inform your OB-GYN about any dental infections or planned procedures.
– Bring a list of all medications, supplements, and prenatal vitamins.
Key Takeaways: Stay Safe and Pain-Free

- Hormonal changes, vomiting, and cravings increase your risk—be proactive.
- Saltwater rinses, clove oil, and cold compresses offer safe temporary relief.
- Acetaminophen (Tylenol) is the only recommended OTC painkiller.
- Dental care is safe in all trimesters—especially cleanings and fillings.
- The second trimester is ideal for non-emergency treatments.
- X-rays and local anesthesia are safe with proper protection.
- Penicillin and amoxicillin are safe antibiotics—avoid tetracyclines.
- Never ignore swelling, fever, or pus—these can harm your baby.
- Prevent problems with daily brushing, flossing, and good nutrition.
- Always talk to both your dentist and OB-GYN before treatment.
Your oral health is part of your prenatal care. By acting early and safely, you protect both yourself and your baby. Don’t suffer in silence—relief is possible, and help is within reach.