Tooth decay affects nearly 2.3 billion people worldwide, making it one of the most common chronic diseases. The good news? Early tooth decay can be reversed—but only if caught before a cavity forms. Once a hole appears in your tooth, natural healing is no longer possible, and dental treatment becomes essential.
The process starts when bacteria in plaque feed on sugars from food, producing acids that strip minerals from your enamel. This is called demineralization. But your body fights back: saliva and fluoride help rebuild weakened enamel through remineralization. When acid attacks happen too often—like from frequent snacking or sugary drinks—demineralization wins, leading to cavities.
This guide walks you through exactly how to fix tooth decay, whether you’re in the early, reversible stage or need professional care. You’ll learn science-backed strategies to reverse white spot lesions, proven ways to prevent further damage, and what to expect from dental treatments when decay progresses. With the right habits and timely action, you can stop decay in its tracks and protect your smile for life.
Decode Early Decay Signs
Spotting tooth decay early is your best chance to reverse it without fillings. Most people miss the warning signs until pain hits—but by then, damage is often advanced.
Identify White Spot Lesions
White spots on your teeth are the first visible sign of enamel demineralization. These chalky areas usually appear near the gumline or between teeth. They’re not cavities yet, but they signal active mineral loss.
- Look for: Faint white or cloudy patches, especially on front teeth
- When to act: Immediately—this stage is fully reversible
- What it means: Acid has begun dissolving calcium and phosphate from enamel
Use a mirror under good lighting to check hard-to-see areas. If you notice white spots, boost your remineralization efforts now. These lesions are your enamel’s cry for help—and with the right response, they can disappear within weeks.
Recognize Hidden Decay
Not all early decay is visible. Some lesions form between teeth or below the gumline, detectable only through dental X-rays or laser scans.
Common hidden signs:
– Lingering sensitivity to cold or sweets
– A rough edge when you run your tongue over a tooth
– Food consistently getting stuck in one spot
If you’ve had past cavities or wear braces, you’re at higher risk. Schedule a dental checkup to catch what you can’t see. Early detection via X-ray can reveal dark spots indicating mineral loss—giving you time to reverse it before drilling begins.
Reverse Early Decay Naturally
Once you spot early damage, act fast. The following science-backed methods can halt and reverse demineralization—before a cavity forms.
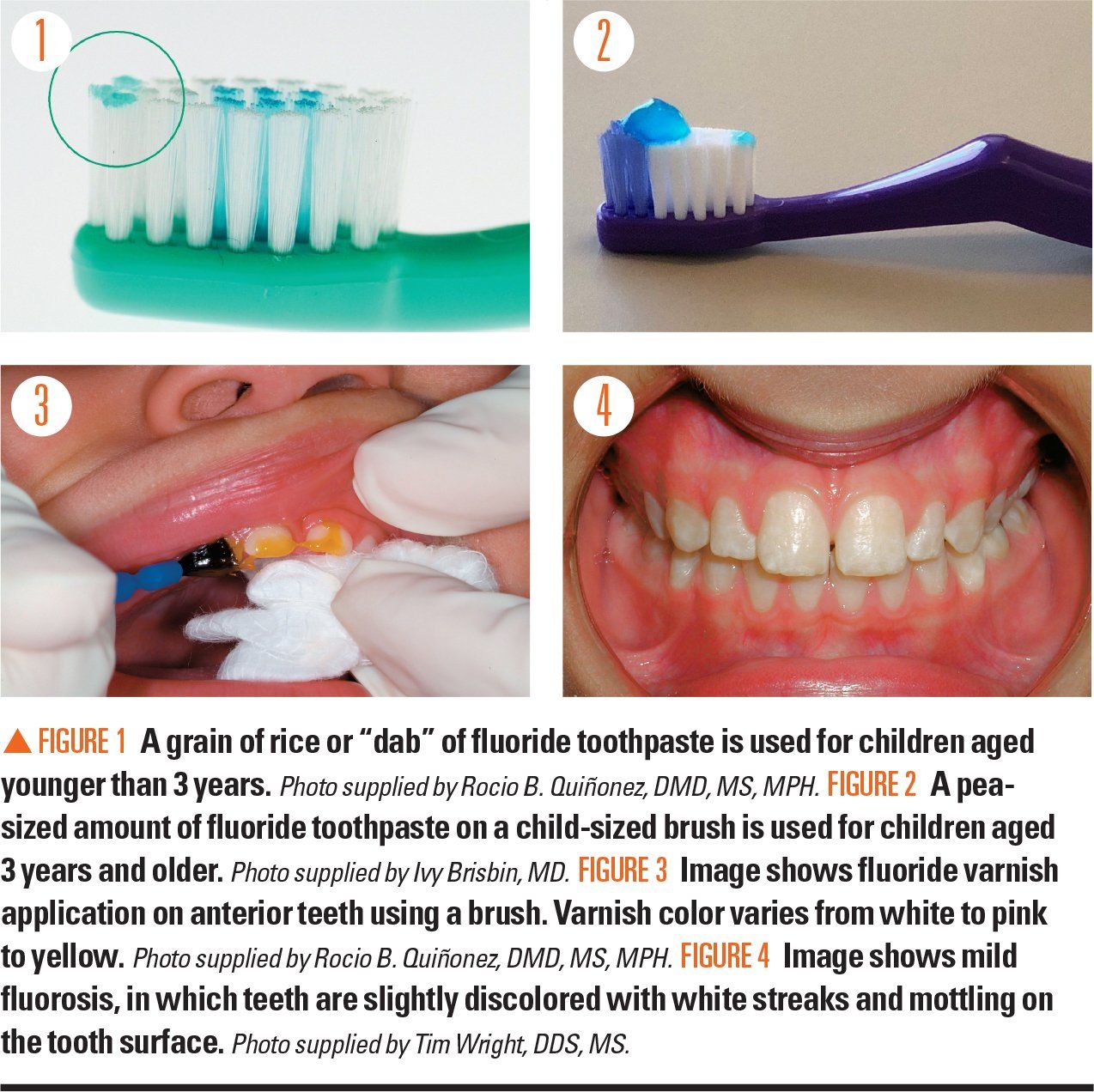
Boost Fluoride Exposure
Fluoride is the gold standard for reversing early tooth decay. It integrates into weakened enamel, forming fluorapatite, a stronger, acid-resistant mineral.
Daily routine:
– Brush twice daily with fluoride toothpaste (1,000–1,500 ppm)
– Spit—don’t rinse—after brushing to leave protective fluoride on teeth
– Use a fluoride mouthwash (0.05% sodium fluoride) once daily
Professional options:
– Ask your dentist for fluoride varnish—applied every 3–6 months
– Consider silver diamine fluoride (SDF) if you can’t get immediate treatment (turns decay black but stops progression)
Tip: Most bottled water lacks fluoride. If you drink only bottled water, talk to your dentist about supplements.
Optimize Your Diet for Remineralization
Food fuels both decay and healing. What you eat directly impacts your mouth’s pH and mineral balance.
Cut these:
– Sugary snacks and drinks (soda, juice, candy)
– Frequent eating (more than 3 meals + 2 snacks/day)
– Sticky carbs (chips, crackers, dried fruit)
Add these:
– Cheese, yogurt, and milk (raise pH, deliver calcium)
– Crunchy vegetables (celery, carrots—clean teeth and stimulate saliva)
– Nuts and seeds (rich in magnesium and healthy fats)
Pro tip: Eat cheese after sugary meals—it neutralizes acid and boosts remineralization.
Stimulate Saliva Flow Daily
Saliva is your mouth’s natural repair system. It washes away food, neutralizes acid, and delivers calcium and phosphate to enamel.
Ways to increase saliva:
– Chew xylitol gum 5–6 times a day for 5–20 minutes
– Stay hydrated—drink water throughout the day
– Suck on sugar-free lozenges if you have dry mouth
Xylitol is key—it blocks Streptococcus mutans, the main bacteria behind cavities, from producing acid.
Balance Oral pH Naturally
An acidic mouth (below pH 5.5) dissolves enamel. Neutral or alkaline conditions support remineralization.
Do this:
– Avoid sipping soda, coffee, or citrus juice all day
– Use a straw for acidic drinks
– Rinse with water after eating or drinking (but wait 30 minutes before brushing)
Try green tea: It contains catechins that fight harmful bacteria and reduce inflammation—without eroding enamel like coffee.
Add Probiotics and Key Nutrients
A healthy oral microbiome crowds out decay-causing bacteria.
Eat more:
– Kefir, kimchi, sauerkraut (probiotics)
– Fatty fish (salmon, sardines—rich in vitamin D)
– Leafy greens (kale, collards—high in calcium and magnesium)
Vitamin D helps your body absorb calcium. Studies show deficiency increases cavity risk by up to 50%.
Stop Decay from Spreading
Even if you can’t reverse it, stopping progression buys time for treatment and prevents new cavities.
Break the Acid Attack Cycle
Each time you eat sugar, plaque bacteria produce acid for 20–30 minutes. Frequent snacking means non-stop attacks.
Fix it:
– Limit eating to 3 meals + 1–2 snacks per day
– Choose low-sugar options (nuts, cheese, veggies)
– Drink water between meals
Warning: “Healthy” snacks like granola bars and fruit juices are often high in hidden sugars. Check labels.
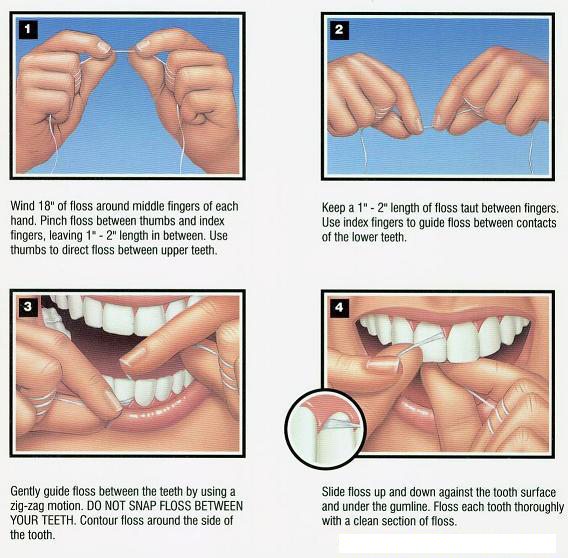
Clean Plaque from Vulnerable Areas
Plaque builds up in grooves, between teeth, and at the gumline—prime spots for decay.
Best cleaning routine:
– Brush for 2 minutes, twice daily, using a soft brush
– Angle bristles at 45 degrees to reach the gumline
– Floss daily—especially between back teeth
– Use an interdental brush if you have braces or gaps
Visual cue: After brushing, swipe your tongue over your teeth. They should feel smooth and clean.
Professional Treatments for Cavities
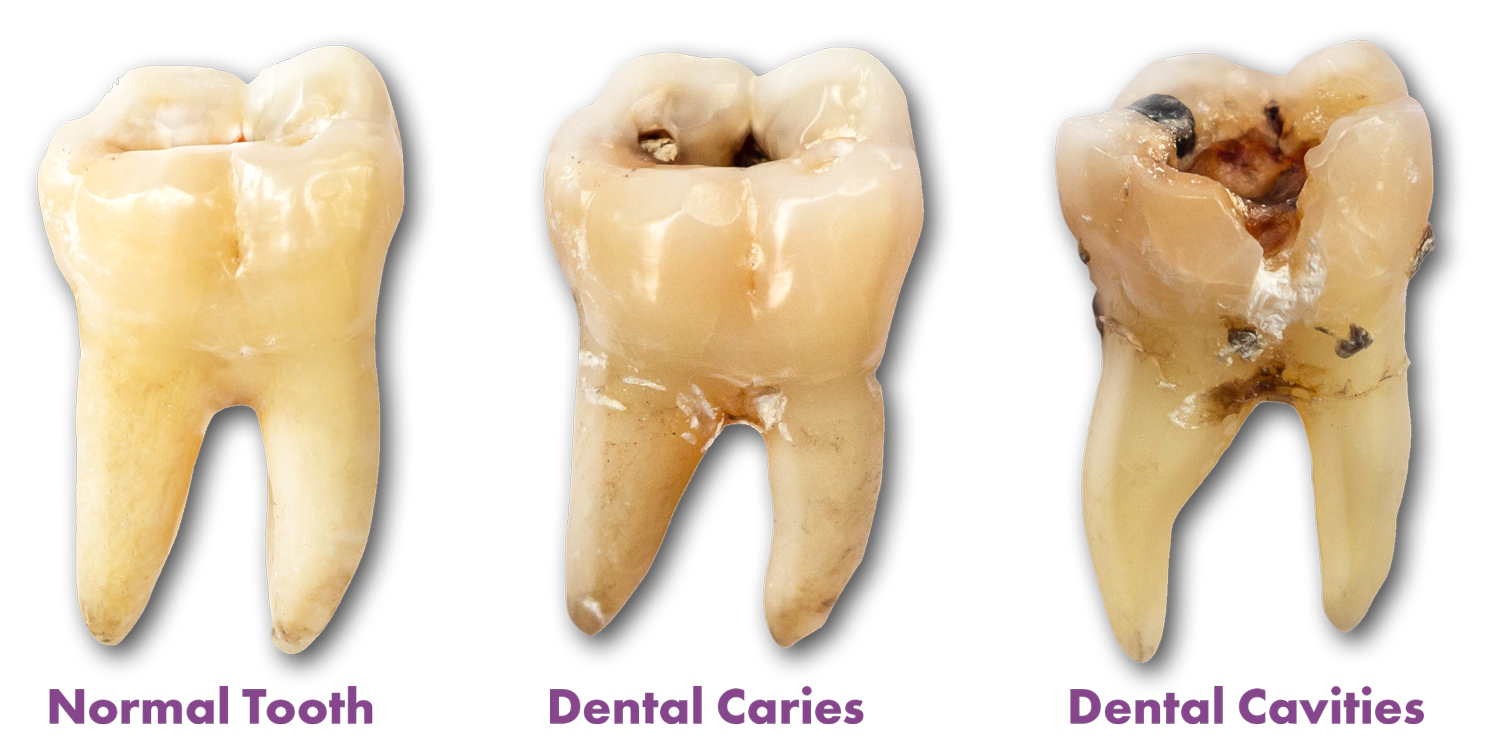
Once a cavity forms—a visible hole or brown/black spot—only a dentist can fix it. Natural methods won’t rebuild lost tooth structure.
Get a Dental Filling
Fillings remove decay and restore the tooth.
Process:
1. Dentist numbs the area (if needed)
2. Removes decayed enamel and dentin with a drill
3. Fills the space with composite (tooth-colored) or amalgam (silver)
Recovery: Mild sensitivity for 1–3 days. Avoid chewing on that side until numbness wears off.
Material choice: Composite looks natural but may wear faster. Amalgam lasts longer but is visible.
Consider Dental Sealants
Sealants are clear or white coatings applied to molar grooves to prevent decay.
Who should get them:
– Children (ages 5–14) when permanent molars erupt
– Adults with deep grooves or high cavity risk
Effectiveness: Up to 80% reduction in pit-and-fissure cavities.
Longevity: Lasts 5–10 years with good care.
Treat Dentin Decay with a Crown
If decay reaches the dentin and weakens the tooth, a filling may not be enough.
When you need a crown:
– Large cavity compromising tooth strength
– Cracked or fractured tooth
– After root canal treatment
Procedure:
– Tooth is reshaped
– Custom crown (porcelain, zirconia, or metal) is cemented over it
– Takes 1–2 visits
Outcome: Restores function and prevents breakage.
Fix Pulp Infection with Root Canal
Deep decay that reaches the pulp causes intense pain and infection.
Symptoms:
– Throbbing toothache
– Pain when biting
– Swelling or gum boil
Root canal steps:
1. Remove infected pulp
2. Clean and disinfect root canals
3. Seal the space
4. Place a crown
Myth: Root canals are painful. In reality, they relieve pain and save the natural tooth.
Handle Abscesses Immediately
An abscess is a dental emergency. Pus at the root tip can spread infection to your jaw or bloodstream.
Signs:
– Severe, constant pain
– Facial swelling
– Fever
– Pimple-like bump on the gum
Treatment:
– Drain the abscess
– Perform root canal or extraction
– Prescribe antibiotics if infection has spread
Act fast: Delay increases risk of systemic complications.
Prevent Future Decay
Once you’ve fixed tooth decay, protect your teeth from recurring damage.
Maintain a Strong Oral Routine
Prevention beats treatment every time.
Daily must-dos:
– Brush 2x/day with fluoride toothpaste
– Floss once daily
– Use fluoride mouthwash (optional)
– Replace toothbrush every 3 months
Night tip: Don’t eat or drink (except water) after brushing at night—this gives saliva uninterrupted time to repair.
Schedule Regular Dental Checkups
Most decay starts between teeth—invisible without X-rays.
Visit every:
– 6 months: Low-risk adults
– 3–4 months: High-risk (dry mouth, braces, past cavities)
What to expect:
– Professional cleaning
– X-rays to detect hidden decay
– Fluoride treatment if needed
– Oral cancer screening
Manage Dry Mouth
Saliva protects your teeth. Low flow (xerostomia) increases decay risk.
Causes:
– Medications (antihistamines, antidepressants)
– Medical conditions (Sjögren’s syndrome, diabetes)
– Radiation therapy
Solutions:
– Chew xylitol gum
– Use saliva substitutes (Biotene)
– Stay hydrated
– Avoid alcohol-based mouthwashes
Special Cases and FAQs
Can You Reverse a Cavity Naturally?
No. Once a hole forms, natural healing is impossible. But white spot lesions—early demineralization—can be reversed with fluoride, diet, and hygiene.
Does Tooth Decay Spread?
Yes. Decay can:
– Move from one tooth to another through shared plaque
– Spread from person to person via saliva (e.g., sharing utensils with infants)
Avoid sharing toothbrushes, cups, or food with young children.
Can You See Decay on an X-ray?
Yes. X-rays show:
– Decay between teeth
– Damage under fillings
– Early lesions not visible to the eye
Dark spots indicate mineral loss—your dentist uses these to plan treatment.
What Does Decay Look Like?
- Early: White or chalky spots
- Moderate: Brown or black discoloration
- Advanced: Visible holes, pits, or crumbling edges
Can Decay Cause Other Health Problems?
Yes. Untreated decay may lead to:
– Abscesses and systemic infections
– Heart disease and stroke (linked to chronic inflammation)
– Diabetes complications
– Pregnancy issues (preterm birth, low birth weight)
Oral health is overall health.
Key Takeaways: Stop Decay Before It Starts
- Early decay (white spots) can be reversed with fluoride, diet, and saliva support.
- Once a cavity forms, only a dentist can fix it—fillings, crowns, or root canals.
- Fluoride is your best defense—use it daily in toothpaste and at dental visits.
- Limit sugar and snacking to reduce acid attacks.
- Floss daily and visit your dentist every 6 months for early detection.
- Dry mouth increases risk—treat it with xylitol, hydration, and saliva aids.
- Children and older adults need extra care—watch for root decay and early cavities.
Tooth decay isn’t inevitable. With the right habits, you can reverse early damage, avoid painful procedures, and keep your natural teeth for life. Start today—your smile depends on it.