You’ve just left the dentist’s office with a new filling, expecting relief—but instead, you’re greeted by sharp zings, a dull ache, or even throbbing pain. You’re not alone. Tooth pain after a filling is surprisingly common, affecting countless patients who’ve undergone routine cavity treatment. While mild sensitivity is normal and typically fades within days, persistent or severe discomfort can be distressing and disruptive.
Most post-filling pain stems from temporary nerve irritation, a high bite, or sensitivity to temperature changes. The good news? With the right approach, you can manage and often eliminate discomfort at home. But knowing when to act—and when to call your dentist—is key. Ignoring warning signs can lead to complications like irreversible pulpitis, infection, or tooth damage. In this guide, you’ll learn how to identify the cause of your pain, apply fast-acting relief strategies, and know exactly when professional help is needed.
Identify the Root Cause of Your Pain
Understand the Most Common Triggers
Not all tooth pain after a filling is the same. Pinpointing the source helps you respond effectively. Tooth sensitivity is the top culprit, especially with deep fillings or composite (tooth-colored) materials. Drilling exposes microscopic dentin tubules that connect directly to the nerve, making your tooth reactive to cold, heat, or even air. This type of discomfort usually improves over 2–4 weeks as the nerve settles.
A high bite—where the filling sits slightly too high—can cause sharp pain when chewing. It feels like “biting on a pebble,” even with minimal misalignment. This excess pressure irritates the ligament around the tooth root and is one of the easiest fixes: your dentist can adjust it in minutes.
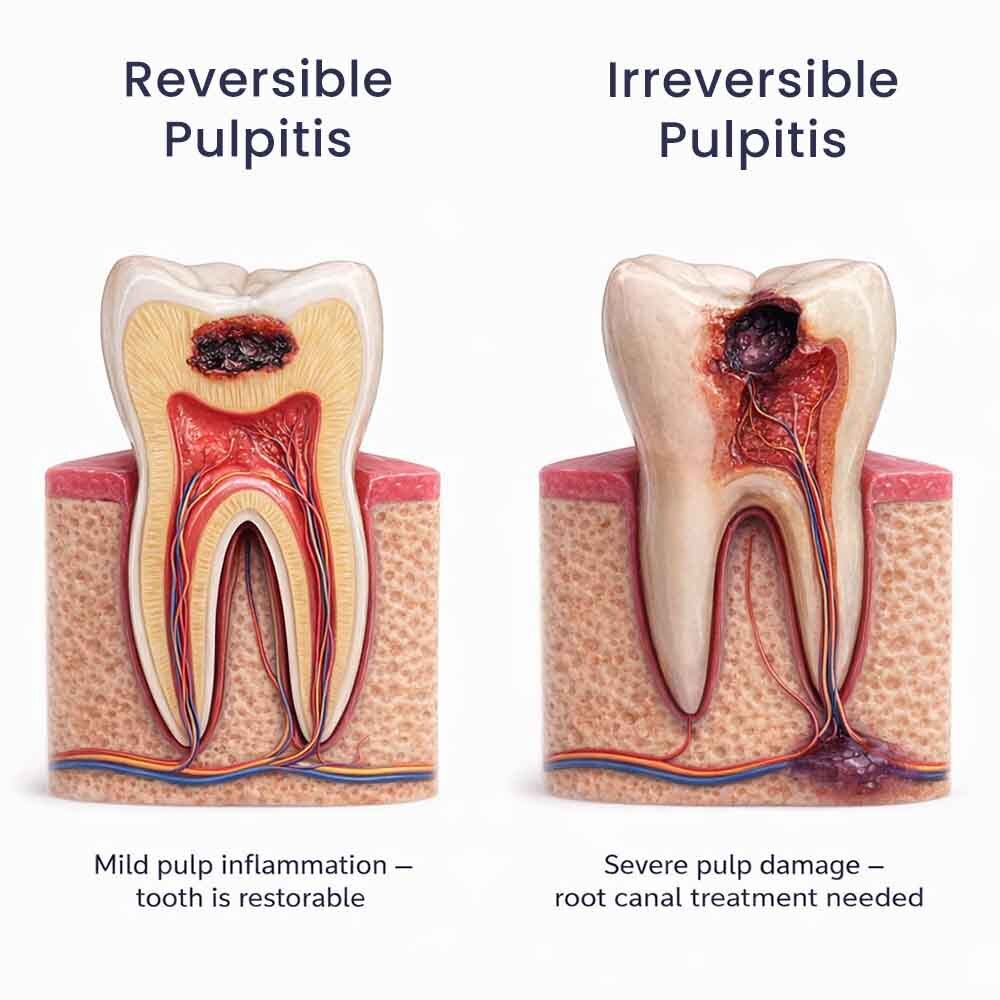
Pulp inflammation (pulpitis) occurs when the nerve is irritated. If pain is brief and only happens with cold, it’s likely reversible and will fade. But if it lingers after the trigger is gone, wakes you at night, or occurs spontaneously, it may be irreversible—and require a root canal.
Rarely, allergic reactions to materials (like amalgam or composite) cause burning, itching, or swelling. Cracked teeth, leaky fillings, or jaw soreness from holding your mouth open can also mimic tooth pain. Accurate diagnosis starts with observing your symptoms closely.
Know When to Seek Immediate Dental Care
Some symptoms are red flags. Throbbing or pulsating pain, especially when lying down, suggests active inflammation or infection—possibly irreversible pulpitis or an abscess. Swelling, fever, or pus around the tooth means infection is present and needs urgent treatment.
If pain lasts longer than 2–4 weeks, worsens over time, or doesn’t respond to over-the-counter meds, it’s not normal healing. Radiating pain to your jaw, ear, or other teeth may indicate nerve involvement. A chipped, cracked, or loose filling, or dark lines around the restoration, could signal decay returning or a failing seal.
Spontaneous pain—occurring without triggers—is often a sign of irreversible nerve damage. While mild sensitivity is expected, persistent or severe symptoms are not part of standard recovery. If you notice any of these warning signs, contact your dentist right away. Delaying care can lead to tooth loss or more complex treatment.
Immediate Relief Strategies You Can Try at Home
Avoid Temperature Extremes
One of the fastest ways to reduce post-filling pain is to avoid hot and cold triggers. Ice cream, iced drinks, coffee, and soup can set off sharp zings in a sensitive tooth. Temperature changes cause the filling and tooth to expand or contract, stimulating exposed dentin and irritating the nerve.
Stick to lukewarm or room-temperature foods and drinks, especially in the first 48 hours. One patient reported nearly complete relief just by switching to meals at body temperature. This simple step reduces nerve stimulation and gives your tooth time to stabilize.
If you must drink something cold, use a straw and direct it away from the filled tooth. And never chew on ice—it adds mechanical stress and extreme cold, worsening sensitivity. Over time, as the nerve calms and dentin seals, you’ll regain tolerance. But during early healing, keeping things neutral is key.
Switch to a Soft, Non-Irritating Diet
What you eat matters just as much as temperature. Hard, sticky, acidic, or sugary foods can aggravate your tooth and delay healing. Nuts, chips, hard candies, and raw veggies put pressure on the filling. Sticky foods like caramel or gum can pull at the restoration, risking dislodgement.
Acidic foods—citrus, soda, wine—can erode enamel and increase sensitivity. Sugar feeds bacteria, raising the risk of new decay around the filling. Instead, choose soft, bland foods that require little chewing: mashed potatoes, scrambled eggs, yogurt, smoothies, soups, and pasta.
Eating on the opposite side of your mouth also helps. Avoid using the filled tooth for at least 24–48 hours. This reduces pressure and lets the tooth settle. If pain flares when you chew, it could be a sign of a high bite—don’t ignore it. A soft diet supports healing and prevents turning a minor issue into a major one.
Use Cold Compresses for External Relief
If your face feels tender or swollen near the filled tooth, a cold compress can help. Apply it to the outside of your cheek for 15 minutes at a time, with 15-minute breaks in between. Do this for the first 24–48 hours.
Cold therapy constricts blood vessels, reducing inflammation and numbing the area. Wrap ice in a clean cloth—never apply it directly to the skin to avoid frostbite. This won’t fix internal tooth pain, but it can ease muscle soreness from holding your jaw open during the procedure.
This is especially useful if you’re also dealing with jaw fatigue or TMJ discomfort. Combine it with rest and gentle jaw stretches to speed recovery. While cold packs won’t cure nerve pain, they’re a safe, effective way to reduce surface discomfort and swelling.
Effective Over-the-Counter and Topical Treatments
Choose the Right Pain Reliever
For quick relief, ibuprofen (Advil, Motrin) is often the best choice. As a nonsteroidal anti-inflammatory drug (NSAID), it reduces both pain and inflammation—key factors in post-filling discomfort. A typical dose is 200–400 mg every 6 hours, not exceeding 1200–2400 mg per day unless directed by a doctor.
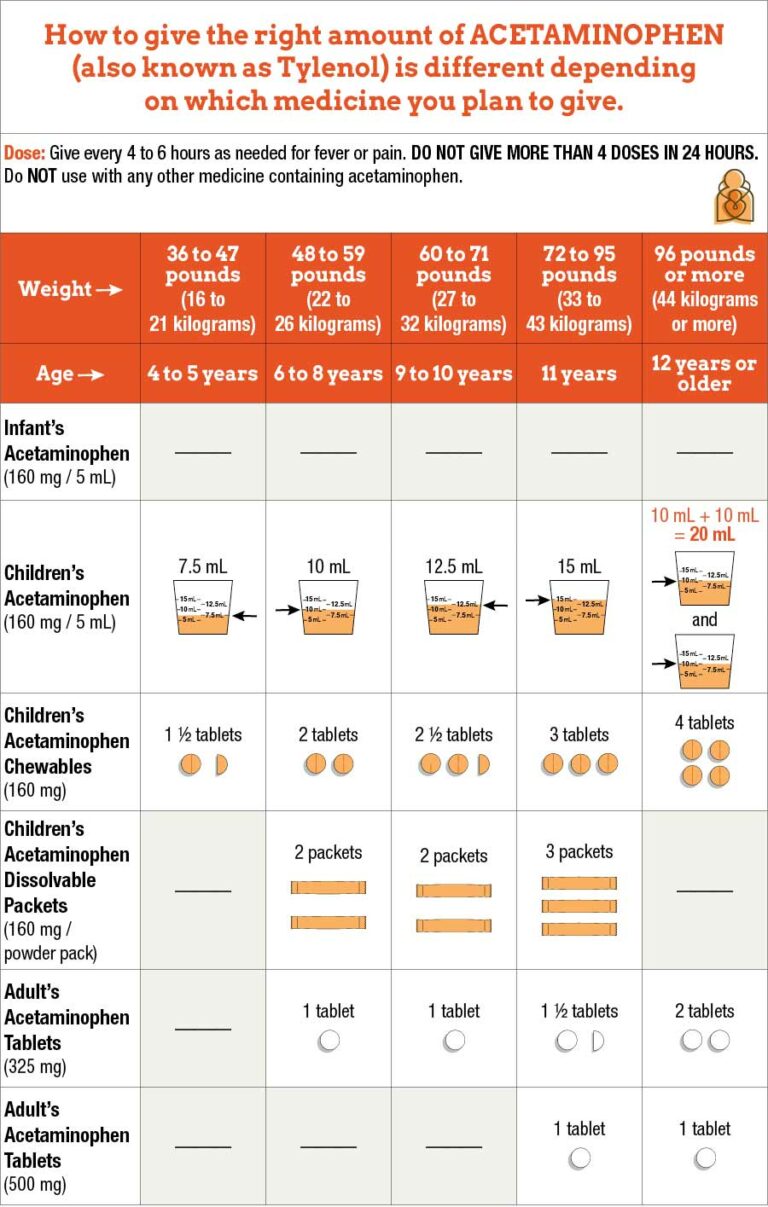
If you can’t take NSAIDs due to stomach issues or medication interactions, acetaminophen (Tylenol) is a solid alternative. It doesn’t reduce inflammation but effectively blocks pain signals. Dose: 500–1000 mg every 6 hours, up to 3000–4000 mg daily.
For stubborn pain, some dentists recommend alternating ibuprofen and acetaminophen every 3 hours (e.g., ibuprofen at 9 AM, Tylenol at 12 PM, ibuprofen at 3 PM). This combo can provide stronger relief without exceeding safe limits—but only under professional guidance.
Never place aspirin directly on the gums—it can cause chemical burns. And avoid alcohol while taking pain meds. Take your first dose at the first sign of discomfort, not after pain peaks, for best results.
Use Desensitizing Toothpaste for Lasting Relief
If sensitivity lingers, desensitizing toothpaste can make a big difference. Brands like Sensodyne, Colgate Sensitive, and Crest Sensi-Relief contain active ingredients that block pain signals. Potassium nitrate calms the nerve, while stannous fluoride seals exposed dentin tubes.
Use it twice daily. After brushing, don’t rinse immediately—spit out excess and let the paste sit on your teeth for maximum effect. For extra relief, apply a dab directly to the sensitive tooth before bed and leave it on overnight.
Some patients start using desensitizing toothpaste a few days before their filling if they’re prone to sensitivity. It takes about 2–4 weeks of consistent use to see full results. While it won’t fix a high bite or infection, it’s a powerful tool for managing normal post-op sensitivity.
Rinse with Saltwater or Fluoride Mouthwash
A warm saltwater rinse is a simple, effective way to soothe irritation and support healing. Mix ½ teaspoon of salt in 8 ounces of warm water. Swish gently for 30 seconds, focusing on the affected area. Spit—don’t swallow. Repeat 2–3 times daily, especially after meals.
Saltwater cleanses the area, reduces bacteria, and eases gum inflammation. It’s ideal for mild soreness or if your gums were irritated during the procedure.
For longer-term protection, use an over-the-counter fluoride mouthwash like ACT or Listerine Total Care. Fluoride strengthens enamel and helps seal open dentin tubules, reducing sensitivity over time. Use it once daily, preferably at night, after brushing.
Natural Remedies for Temporary Relief
Apply Clove Oil for Fast Numbing
Clove oil is a time-tested natural remedy for tooth pain. Its active ingredient, eugenol, is a natural anesthetic and antiseptic used in dental cements and temporary fillings. It numbs the area and reduces inflammation.
To use: Soak a cotton swab in clove oil and dab it gently on the painful tooth or gum. Avoid swallowing—use sparingly. You can repeat every few hours as needed.
Some people mix a few drops with a carrier oil like coconut oil to dilute it. While clove oil won’t cure an infection or fix a high filling, it provides fast, temporary relief when pain strikes. Keep it on hand for emergencies—but don’t rely on it for persistent issues.
Try Peppermint Tea or Vanilla Extract
Other kitchen remedies offer mild relief. Peppermint tea bags, cooled and placed on the tooth, can numb the area thanks to menthol’s cooling effect. Hold it in place for 10–15 minutes.
Vanilla extract contains alcohol and natural compounds that may soothe nerves. Dab a small amount on a cotton ball and apply to the tooth. While evidence is anecdotal, many report a calming effect.
These methods are best for mild discomfort and should complement—not replace—standard care. They’re safe, accessible, and can help you get through the night until you can see your dentist.
Professional Solutions for Persistent Pain
Get a Bite Adjustment
If pain happens only when biting down, you likely have a high filling. This is one of the most common—and easiest—causes of post-filling pain. Your dentist uses articulating paper to see where your teeth hit too hard, then smooths the filling with a drill. The adjustment takes minutes and often brings immediate relief.
Don’t suffer hoping it will “wear down” on its own. A high bite can lead to inflammation, cracked teeth, or TMJ issues. Call your dentist if you feel your bite is “off.” Most practices will fix this at no extra cost, even weeks later.
Replace or Repair a Faulty Filling
If your filling is cracked, chipped, or leaking, it may need replacement. Bacteria can seep under it, causing decay and pain. Your dentist will remove the old filling, clean the area, and place a new one.
In cases of secondary decay, more tooth structure may need removal. The new filling might be larger—or a crown may be needed if the tooth is weak. Glass ionomer or ceramic fillings may be recommended for less sensitivity.
Consider Root Canal Therapy
If you have spontaneous, lingering pain, especially at night, you may need a root canal. This treats irreversible pulpitis or infected pulp. The procedure removes the damaged nerve, cleans the canals, and seals them. A crown is usually placed afterward.
Contrary to myths, root canals relieve pain—they don’t cause it. Without treatment, infection can spread, leading to abscess or tooth loss. If your dentist recommends one, don’t delay. It saves your tooth and ends the pain.
Final Note: Most tooth pain after a filling fades within days. Use home remedies, OTC meds, and smart habits to manage discomfort. But if pain lasts more than 2–4 weeks, is severe, or comes with swelling or fever, see your dentist. A quick adjustment or treatment can save you from bigger problems. Don’t suffer in silence—your dentist wants to help.