If you’re feeling a jolt of pain every time you sip coffee, bite down, or even breathe in cold air, you may have an exposed tooth nerve. This condition isn’t just uncomfortable—it’s a warning sign that your tooth’s inner nerve is under attack. Unlike minor sensitivity, an exposed nerve won’t heal on its own and can lead to infection, abscesses, or even tooth loss if ignored. The good news? You’re not powerless. While professional dental treatment is essential, there are immediate, effective steps you can take at home to reduce pain and protect your tooth until you get help. This guide will show you how to recognize the signs, find fast relief, understand treatment options, and prevent future damage—so you can act quickly and confidently.
Recognize the Symptoms Early
Sharp or Throbbing Tooth Pain
A sudden, stabbing pain when you chew or a constant throb that won’t go away is one of the clearest signs of nerve exposure. This isn’t fleeting discomfort—it’s persistent and often worsens at night when lying down increases blood flow to the head. If the pain lingers long after you’ve stopped eating or drinking, it likely means the pulp (the nerve center of your tooth) is inflamed or infected. Unlike regular tooth sensitivity, nerve-related pain doesn’t fade quickly—it’s a red flag that deeper damage has occurred.
Extreme Sensitivity to Temperature
Do hot soups or iced drinks make you wince? Prolonged sensitivity to heat and cold is a hallmark of an exposed nerve. Healthy teeth react briefly to temperature changes, but when dentin or pulp is exposed, the sensation becomes intense and long-lasting. This happens because tiny channels called dentinal tubules connect the outer tooth to the nerve. When these are open due to enamel loss or cracks, stimuli travel straight to the nerve, triggering sharp pain.
Pain When Chewing or Biting
Discomfort during chewing often points to structural damage like a crack or deep decay. You might feel pain when releasing the bite—this “rebound pain” is a classic sign of a hairline fracture. Avoid using that side of your mouth to prevent further damage, and don’t ignore it. What starts as mild discomfort can quickly escalate into severe nerve pain or tooth fracture.
Visible Damage or Discoloration
Take a close look at the painful tooth. Are there dark spots, chips, or cracks? A brown or black area could indicate advanced decay, while a grayish tint may mean the nerve has died—a condition called pulp necrosis. Even if the pain stops, this isn’t a good sign. A dead nerve can still harbor bacteria, leading to abscesses and swelling.
Swelling or Pus Around the Gum
Swelling near the base of a tooth, along with a bad taste or foul smell, signals a serious infection. Pus draining from the gum means a dental abscess has formed. This is a dental emergency. Left untreated, the infection can spread to your jaw, neck, or even bloodstream, posing life-threatening risks.
Immediate Home Relief Methods
Use a Saltwater Rinse
Swish warm saltwater (½ to 1 tsp salt in 8 oz of water) for 30 seconds, 2–3 times daily. This simple rinse reduces inflammation, flushes out debris, and creates a less acidic environment in your mouth. It’s especially helpful after trauma or if food is trapped near the damaged tooth.
Apply a Cold Compress
Place an ice pack wrapped in a cloth on your cheek over the painful area for 15–20 minutes. The cold numbs local nerves and reduces swelling. Never apply ice directly to the tooth—this can worsen sensitivity.
Take OTC Pain Relievers
Ibuprofen (Advil, Motrin) is ideal because it fights both pain and inflammation. Take 200–400 mg every 6 hours as needed. Acetaminophen (Tylenol) works well for pain but doesn’t reduce swelling. Some people alternate between the two every 3 hours for stronger relief—just consult your doctor first.
Warning: Never place aspirin or other pills directly on the gum or tooth. This can burn soft tissues and delay healing.
Try Clove Oil for Natural Numbing
Dab 1–2 drops of clove oil (eugenol) on a cotton swab and apply gently to the affected area. Clove oil acts as a natural anesthetic and antimicrobial. Reapply every few hours, but avoid overuse, which can irritate gums.
Use Desensitizing Toothpaste
Brush with a toothpaste like Sensodyne or Colgate Sensitive. These contain potassium nitrate or stannous fluoride, which block pain signals from the nerve. Use twice daily—results build over 2–4 weeks. Avoid whitening formulas, which are abrasive and may worsen exposure.
Apply Topical Oral Anesthetics
Products like Orajel or Anbesol (with benzocaine or lidocaine) provide quick, short-term numbing. Apply a small amount directly to the tooth and gum with a cotton swab. Effective for 15–30 minutes, but not safe for children under 2 due to rare risks.
Adjust Your Diet Immediately
Stop eating:
– Hot, cold, or sugary foods
– Acidic drinks like soda or citrus juice
– Hard, crunchy, or sticky items
Instead, choose lukewarm, soft foods like mashed potatoes, yogurt, or oatmeal. Rinse your mouth after meals to keep the area clean.
Important: These remedies only ease symptoms—they don’t fix the problem. See a dentist as soon as possible.
See a Dentist: What to Expect
Professional Diagnosis Steps
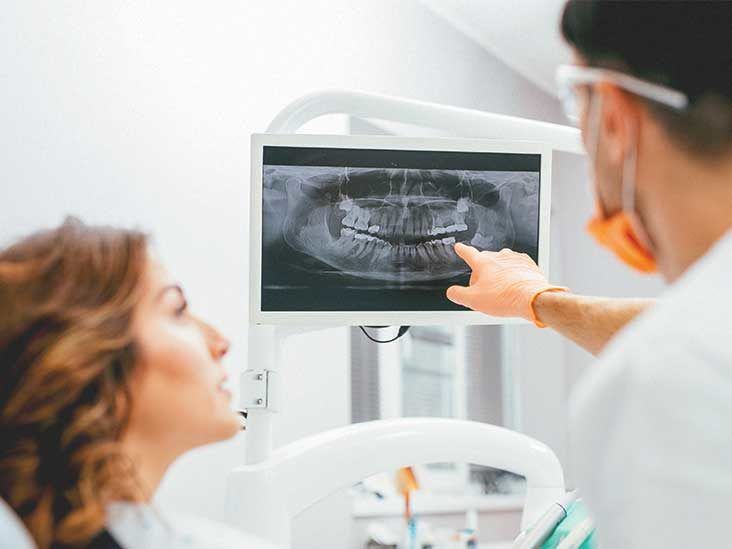
Your dentist will start with a visual exam, checking for decay, cracks, or gum recession. They may tap the tooth (percussion test) to see if it hurts—that suggests pulp inflammation. Cold air or a chilled instrument tests nerve responsiveness. Lingering pain after the cold stimulus means the pulp is likely irreversibly damaged.
X-rays reveal hidden decay, bone loss, or abscesses at the root. In some cases, dye or transillumination (shining a light through the tooth) helps spot tiny cracks.
Electric Pulp Testing (EPT)
This tool sends a mild electrical current to the tooth. A healthy nerve responds at a certain threshold. No response may mean the nerve is dead; an exaggerated response indicates severe inflammation.
Treatments Based on Damage Level

Dental Fillings for Minor Exposure
If decay has reached near the nerve but hasn’t infected it, a filling may suffice. The dentist removes the decay, cleans the cavity, and seals it with composite or amalgam. This stops further irritation and protects the pulp. Success is high if the nerve is still healthy.
Dental Bonding for Small Cracks
For minor enamel defects exposing dentin, bonding uses tooth-colored resin to seal the area. It’s fast, non-invasive, and improves appearance. While it doesn’t reach deep nerve issues, it helps prevent progression.
Root Canal Therapy for Infected Nerves
If the pulp is infected or inflamed beyond repair, a root canal is necessary. Here’s what happens:
1. Local anesthesia numbs the area.
2. A small access hole is drilled into the tooth.
3. The infected pulp is removed from the canals.
4. Canals are cleaned, shaped, and disinfected.
5. Filled with rubber-like gutta-percha.
6. Sealed with a temporary or permanent filling.
Contrary to myths, modern root canals are painless and save the natural tooth. Over 95% succeed long-term.
Dental Crown After Major Repair
After a root canal or large filling, a crown restores strength and function. The tooth is reshaped, an impression is taken, and a custom crown—made of porcelain, zirconia, or metal—is cemented in place. A crown prevents future fractures and lasts 10–15 years with proper care.
Tooth Extraction When Saving Isn’t Possible
If the tooth is too damaged or the infection is uncontrollable, extraction is the safest option. Simple extractions are done under local anesthesia; surgical ones may require sedation. Aftercare is crucial—avoid smoking, spitting, or straws for 48 hours to prevent dry socket.
Replacement options include:
– Dental implants: Titanium post fused to jawbone; most durable
– Bridges: Artificial tooth anchored to adjacent teeth
– Partial dentures: Removable and cost-effective
Gum Grafting for Root Exposure
If gum recession has exposed the root, a gum graft can help. Tissue from your palate or a donor source is grafted over the exposed area. This reduces sensitivity, prevents further recession, and improves gum health.
When to Seek Emergency Care

Signs of a Dental Emergency
Go to a dentist or ER immediately if you have:
– Severe, unrelenting pain
– Facial swelling or puffiness
– Fever or chills
– Difficulty swallowing or breathing
– Pus around the tooth
– A loose or knocked-out tooth
These symptoms suggest a spreading infection, which can become life-threatening.
What to Do If a Tooth Is Knocked Out
- Pick it up by the crown (not the root).
- Rinse gently with milk or saline—don’t scrub.
- Try to reinsert it into the socket.
- If not possible, store it in milk or saliva.
- See a dentist within 30 minutes—reimplantation is possible.
Risks of Delaying Treatment
Dental Abscess Formation
An untreated exposed nerve often leads to a periapical abscess—a pus-filled pocket at the root tip. This causes throbbing pain, swelling, and systemic illness. Drainage and antibiotics are needed, but the tooth still requires a root canal or extraction.
Bone and Tooth Loss
Chronic infection destroys the jawbone supporting the tooth. This weakens adjacent teeth and complicates future implants. In severe cases, the tooth becomes too loose to save and must be removed.
Systemic Health Risks
Oral bacteria can enter the bloodstream, increasing the risk of:
– Heart disease
– Endocarditis
– Complications in diabetes and pregnancy
Even mild dental infections shouldn’t be ignored.
Prevent Future Nerve Exposure
Maintain Excellent Oral Hygiene
Brush twice daily with a soft-bristled toothbrush and fluoride toothpaste. Floss daily and use an antimicrobial mouthwash. Gentle, circular motions protect enamel and gums.
Visit Your Dentist Every 6 Months
Regular cleanings and check-ups catch problems early. X-rays detect hidden decay and cracks before they reach the nerve.
Wear a Mouthguard
Use a custom night guard if you grind your teeth. Wear a sports mouthguard to prevent trauma.
Avoid Harmful Habits
Don’t chew ice, hard candies, or pens. These can chip or crack teeth.
Limit Acidic and Sugary Foods
Rinse with water after eating acidic foods. Wait 30 minutes before brushing.
Use Proper Brushing Technique
Aggressive brushing wears down enamel. Use a 45-degree angle and soft pressure.
Final Note: An exposed tooth nerve won’t heal on its own. While home remedies can ease pain temporarily, only professional dental care can resolve the issue. From fillings to root canals, modern dentistry offers effective, pain-free solutions. The key is acting fast—early treatment saves your tooth, prevents infection, and protects your overall health. Don’t wait for the pain to get worse. If you suspect nerve exposure, call your dentist today. Your smile depends on it.