A loose tooth in an adult is never normal—and it’s often a warning sign of something more serious beneath the surface. While children naturally lose baby teeth, adult tooth mobility points to underlying issues like gum disease, trauma, or grinding. Left untreated, a wobbly tooth can lead to pain, infection, and even permanent tooth loss.
The good news? Many loose teeth can be stabilized or saved—if you act quickly. Whether the cause is periodontal disease, injury, or bruxism, effective treatments exist. From professional dental procedures like deep cleaning and splinting to supportive home care like saltwater rinses and proper nutrition, this guide covers everything you need to know.
You’ll learn how dentists diagnose the severity of tooth looseness, what treatments actually work, and how to prevent future problems. No fluff, no generic advice—just clear, actionable steps based on dental science. If your tooth feels loose, read on. Your smile depends on it.
Identify the Cause of Looseness
Before any treatment, it’s crucial to understand why your tooth is loose. The approach differs significantly depending on whether the cause is gum disease, trauma, or grinding. Misdiagnosing the problem at home can delay healing and worsen damage.
Gum Disease and Bone Loss
Periodontitis is the leading cause of loose adult teeth. Plaque builds up along the gumline, hardens into tartar, and triggers inflammation. Over time, this infection spreads below the gums, destroying the bone and ligaments that hold teeth in place.
As bone resorbs, the tooth loses support and begins to shift. Early signs include bleeding gums, bad breath, and gum recession. Without treatment, mobility increases—and so does the risk of tooth loss.
Trauma or Impact Injury
A fall, sports collision, or even biting down hard on something can jar a tooth loose. The periodontal ligament—the fibrous tissue anchoring the tooth to the bone—can stretch or tear. In mild cases, the ligament heals on its own. In severe cases, the tooth may need splinting or even extraction.
Even if there’s no visible damage, internal injury to the root or surrounding bone can still occur. That’s why any post-trauma looseness requires immediate dental evaluation.
Teeth Grinding (Bruxism)
Grinding or clenching—especially at night—puts extreme pressure on teeth. This parafunctional force wears down enamel, stresses the supporting bone, and can gradually loosen teeth over time.
Many people don’t realize they grind until they notice symptoms: jaw pain, headaches, or a loose tooth. If bruxism is the culprit, treating it is essential to prevent further damage.
Assess Tooth Mobility Level

Dentists classify tooth movement on a three-tier scale. Knowing where your tooth falls helps determine if it can be saved—or if extraction is unavoidable.
Class I: Slight Movement
The tooth moves less than 1 millimeter when pushed side to side. This mild mobility may resolve with improved oral hygiene and avoiding chewing on that side. Often seen after minor trauma or early gum disease.
Action Step: Stick to a soft diet, practice gentle brushing, and monitor for improvement within a week.
Class II: Moderate Movement
Horizontal movement between 1–2 mm. At this stage, the tooth won’t stabilize on its own. Professional treatment is required to prevent progression.
Action Step: See a dentist immediately. Treatment usually includes splinting and deep cleaning if gum disease is present.
Class III: Severe Mobility
The tooth moves more than 2 mm side to side—or shifts vertically (up and down). This level of looseness typically means extensive bone loss or severe trauma.
Prognosis: Poor. The tooth is often non-salvageable and may need extraction.
Next Step: A dentist will evaluate whether to extract and replace the tooth with an implant, bridge, or denture.
Stop Further Damage Immediately
Once you notice looseness, your actions in the first 24–48 hours can make a big difference. Avoid habits that worsen the condition while you wait for professional care.
Avoid Chewing on the Loose Side
Biting pressure can aggravate an already unstable tooth. Stick to soft foods like yogurt, mashed potatoes, or smoothies. Cut food into small pieces and chew on the opposite side of your mouth.
Pro Tip: Even if it doesn’t hurt, chewing on a loose tooth delays healing and can cause irreversible damage.
Don’t Wiggle the Tooth
It’s tempting to test how loose it is with your tongue or finger—but this only worsens ligament strain. Keep the area undisturbed to give tissues a chance to stabilize.
Use a Soft-Bristled Toothbrush
Brush gently around the loose tooth with a soft-bristled brush. Aggressive scrubbing can irritate gums and accelerate bone loss. Use circular motions, not back-and-forth sawing.
Seek Emergency Dental Care
A loose tooth is a dental emergency. Don’t wait for pain to get worse. Early intervention improves the odds of saving the tooth and prevents complications like infection or abscess.
What to Expect at the Dentist
Your dentist will perform a full assessment, including:
- Visual exam of gums and tooth alignment
- Periodontal probing to measure pocket depth
- X-rays to check bone levels and root health
Based on findings, they’ll recommend one or more treatments tailored to the cause.
Treat Gum Disease with Deep Cleaning
If gum disease is the root cause, scaling and root planing (SRP) is the first-line treatment. It’s often called a “deep cleaning” and is more thorough than a routine dental cleaning.
Scaling: Remove Plaque and Tartar
The dentist or hygienist uses specialized tools to scrape away plaque and tartar from above and below the gumline. This eliminates the bacterial colonies fueling inflammation.
Key Point: Tartar can’t be removed by brushing alone—only a professional can do it safely.
Root Planing: Smooth the Tooth Roots
After scaling, the root surfaces are smoothed to remove rough areas where bacteria hide. This allows the gums to reattach to the tooth, reducing pocket depth and stopping disease progression.
Recovery: Mild sensitivity and gum tenderness may last a few days. Full healing takes 4–6 weeks.
Outcome: Reduced inflammation, tighter gums, and gradual tooth stabilization—especially when combined with improved home care.
Stabilize with Dental Splinting

For moderate to severe mobility, splinting bonds the loose tooth to adjacent stable teeth. This distributes chewing forces and gives the periodontal ligament time to heal.
Temporary vs. Permanent Splints
- Temporary splints: Made of composite resin and wire, worn for weeks to months during healing. Removed once the tooth stabilizes.
- Permanent splints: May involve crowns or custom bars for long-term support. Used when bone loss is significant but the tooth is still functional.
Visual Cue: After splinting, the tooth should feel firm and no longer shift when touched.
Timeframe: Healing can take 4–8 weeks, depending on the cause and severity.
Adjust Your Bite to Reduce Pressure
If bruxism or misaligned teeth are contributing to looseness, your dentist may perform an occlusal adjustment—reshaping the biting surface to balance your bite.
How Bite Adjustment Works
Small amounts of enamel are carefully removed from high-contact areas. This eliminates uneven pressure points that overload specific teeth.
Result: Smoother chewing, reduced stress on the loose tooth, and prevention of further wear.
Note: This is a conservative procedure—only minimal enamel is removed, and it doesn’t require anesthesia in most cases.
Use a Night Guard for Teeth Grinding
If you grind your teeth at night, a custom-fitted night guard is essential. Over-the-counter boil-and-bite guards offer limited protection—custom ones from your dentist fit precisely and last longer.
Benefits of a Custom Night Guard
- Prevents enamel wear
- Reduces strain on jaw muscles
- Protects teeth and supporting bone from grinding forces
Wear Time: Typically worn every night. Long-term use is common for chronic bruxism.
Pro Tip: Combine with stress management techniques—bruxism is often linked to anxiety or poor sleep.
Consider Surgical Options for Severe Cases
When non-surgical treatments aren’t enough, surgery may be needed—especially with advanced bone loss or deep periodontal pockets.
Flap Surgery for Deep Pockets
Also called pocket reduction surgery, this procedure involves lifting the gums to access and clean infected areas beneath.
- Gums are gently folded back
- Tartar and bacteria are removed from roots and bone
- Gums are sutured back into place
Goal: Reduce pocket depth and eliminate infection sources.
Bone Grafting to Restore Support
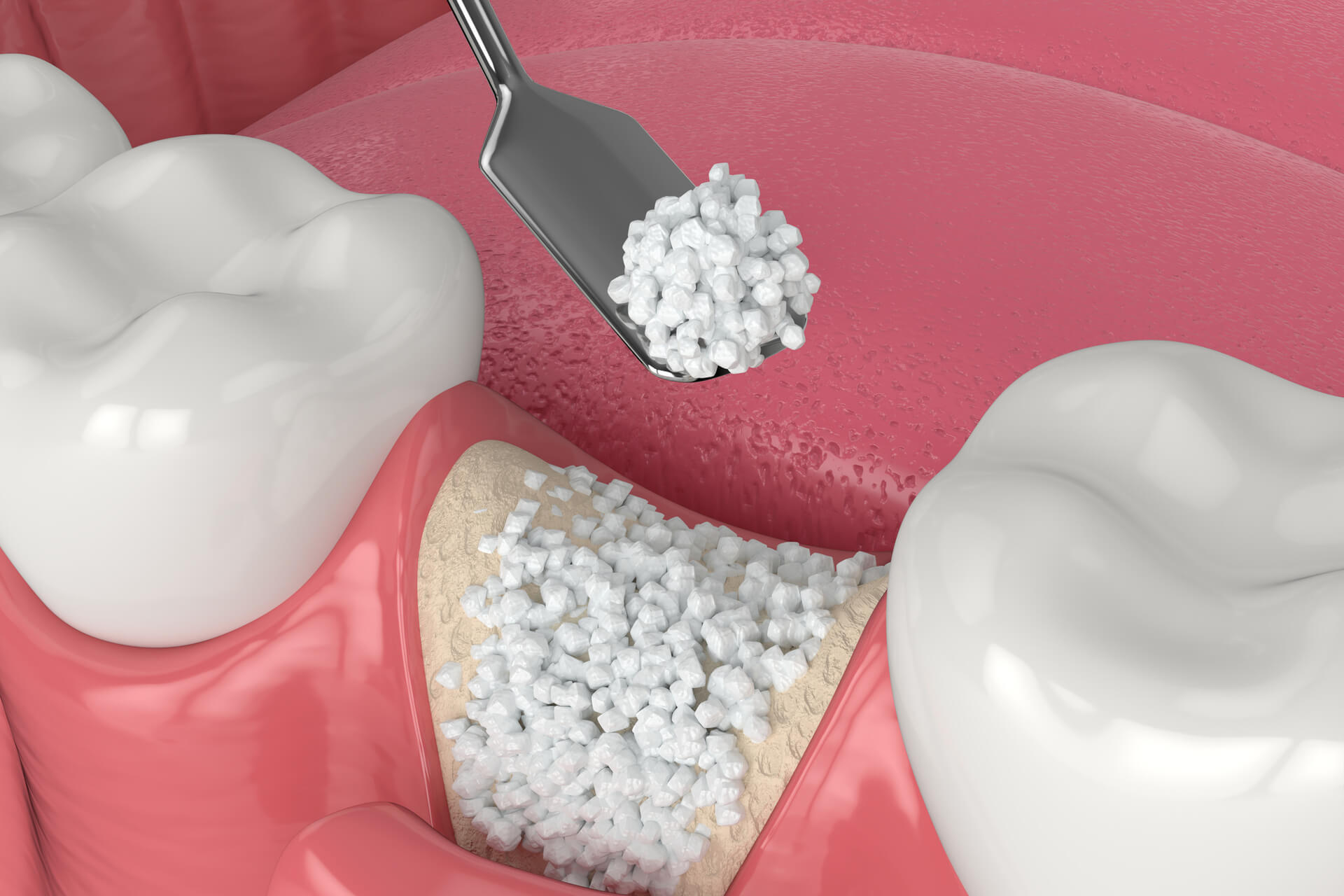
If bone loss has occurred, a graft can rebuild the foundation around the tooth.
- Materials Used: Your own bone, donor bone, or synthetic material
- Process: Graft is placed in the defect to stimulate new bone growth
Healing Time: 3–6 months. Often done alongside guided tissue regeneration.
Guided Tissue Regeneration (GTR)

A biocompatible membrane is placed between the tooth and gum to block soft tissue from filling the space. This allows slower-growing bone and ligament cells to regenerate.
Best For: Teeth with deep, narrow bone defects.
Success Rate: Higher when combined with bone grafts and good oral hygiene.
Soft Tissue Grafts for Receding Gums
Exposed roots from gum recession can contribute to tooth looseness. A soft tissue graft covers the root and strengthens the gum margin.
- Tissue is taken from the palate or a donor source
- Sutured to the receded area
Outcome: Improved gum health, reduced sensitivity, and better tooth stability.
Support Healing with Home Care
While professional treatment is essential, what you do at home plays a key role in recovery. These remedies support healing—but never replace dental care.
Rinse with Warm Saltwater
A simple, effective way to reduce inflammation and kill bacteria.
- How to Use: Dissolve 1 tsp salt in a glass of warm water
- Frequency: Gargle for 30 seconds, 2–3 times daily
Benefits: Natural antiseptic, reduces swelling, speeds healing.
Try a Hydrogen Peroxide Rinse
Kills bacteria and helps prevent secondary infection.
- Mix: Equal parts 3% hydrogen peroxide and water
- Use: Swish for 30 seconds, then spit. Do not swallow.
- Frequency: Once or twice daily
Caution: Don’t overuse—can cause dryness or irritation.
Apply Turmeric and Black Pepper Paste
Turmeric contains curcumin, a powerful anti-inflammatory and antimicrobial compound.
- Recipe: Mix equal parts turmeric powder and black pepper with water
- Apply: Use a clean finger to dab on the affected gum area
- Wait: Leave on for 2–3 minutes, then rinse
Why Black Pepper? It boosts curcumin absorption by up to 2,000%.
Optimize Your Diet for Strong Teeth
Nutrition directly impacts gum and bone health. A nutrient-rich diet supports healing and helps prevent future loosening.
Eat More Calcium and Vitamin D
These work together to strengthen jawbone and tooth support.
- Calcium Sources: Milk, cheese, yogurt, kale, almonds
- Vitamin D Sources: Salmon, egg yolks, sunlight, fortified foods
Tip: Without enough vitamin D, your body can’t absorb calcium effectively.
Boost Vitamin C for Gum Health
Essential for collagen production—the protein that holds gums together.
- Best Sources: Oranges, strawberries, bell peppers, broccoli
- Deficiency Risk: Low vitamin C can lead to scurvy, which causes gum bleeding and tooth loss
Include Phosphorus and Magnesium
- Phosphorus: Works with calcium in bone mineralization (found in meat, fish, beans)
- Magnesium: Supports bone density (found in nuts, seeds, whole grains)
Avoid: Sugary, acidic, or sticky foods that feed harmful bacteria.
Prevent Future Tooth Loosening
Once a tooth has been loose, it’s more vulnerable. Long-term prevention is key to avoiding recurrence.
Visit Your Dentist Every 6 Months
Regular check-ups catch gum disease early—before it causes bone loss. Professional cleanings remove tartar that brushing can’t.
Red Flag: Skipping cleanings increases your risk of periodontitis by 30–50%.
Monitor for Teeth Grinding
Signs include:
– Worn-down or flattened teeth
– Morning jaw soreness
– Headaches upon waking
If you suspect grinding, ask your dentist about a night guard.
Quit Smoking and Limit Alcohol
- Smoking: Reduces blood flow to gums, slows healing, and doubles periodontal disease risk
- Alcohol: Contributes to dry mouth and gum inflammation
Even cutting back helps.
Use Proper Brushing Technique
- Use a soft-bristled brush
- Apply gentle pressure with circular motions
- Replace your toothbrush every 3–4 months
Myth: Hard brushing doesn’t clean better—it damages gums and enamel.
Manage Systemic Health Conditions
Certain medical conditions increase the risk of loose teeth. Controlling them improves oral health.
Control Diabetes
High blood sugar weakens the immune response, making gum infections harder to fight. Diabetics are 2–3 times more likely to develop periodontitis.
Action Step: Keep blood sugar levels in target range and inform your dentist.
Treat Osteoporosis
This bone-weakening disease affects the jawbone too. Postmenopausal women are especially at risk.
Dental Link: Studies show osteoporosis increases tooth loss risk by up to 50%.
Coordination: Work with your doctor and dentist to manage both conditions.