Waking up with a dull, throbbing ache in your upper teeth—especially when you bend forward or lie down—can feel like a dental emergency. But if your dentist finds no cavities, abscesses, or gum disease, the real culprit might not be in your mouth at all. Tooth pain from sinus pressure is surprisingly common and often mistaken for a cavity or tooth infection. This type of discomfort stems not from dental decay, but from inflamed maxillary sinuses pressing on the roots of your upper molars and premolars. These sinuses sit just above your upper teeth and share nerve pathways, so the brain can misinterpret sinus pressure as tooth pain.
The good news? Unlike true dental pain, which may require fillings, root canals, or extractions, sinus-related toothaches typically resolve once the underlying congestion clears—usually within 7 to 14 days. With targeted self-care, you can relieve symptoms fast by treating the root cause: sinus inflammation. This guide will help you identify whether your tooth pain is sinus-related, apply effective home remedies, know when to seek medical help, and prevent future episodes.
Identify the Signs of Sinus Tooth Pain
Recognize the Pattern of Referred Pain
Sinus-related tooth pain has a distinct profile that sets it apart from dental issues. If you’re feeling a dull, aching pressure across multiple upper teeth—especially on both sides of your mouth—and the pain worsens when you lean over or lie flat, your sinuses are likely the source. Unlike a cavity, this pain is rarely sharp or triggered by hot, cold, or sweet foods. Instead, it feels like a constant, radiating pressure in the upper jaw.
Other key indicators include the absence of visible dental damage, such as decay or swollen gums, combined with nasal symptoms like congestion, postnasal drip, or facial fullness. If you’re also experiencing a headache, fatigue, or a reduced sense of smell, it’s more evidence your sinuses—not your teeth—are to blame.
Pro Tip: If your tooth pain improves after using a decongestant or steam inhalation, it’s a strong sign the issue is sinus-related.
Rule Out Dental Problems First
While sinus pressure is a frequent imitator, real dental issues must be ruled out. See a dentist if:
– The pain is isolated to one specific tooth
– You feel sharp pain when chewing or drinking hot or cold liquids
– There’s visible decay, gum swelling, or pus around a tooth
– Sensitivity persists even after your sinus symptoms have cleared
Dental X-rays can detect hidden problems like abscesses, cracked teeth, or deep decay. If your teeth are healthy, the focus should shift to relieving sinus congestion and inflammation.
Reduce Sinus Pressure with Natural Remedies
Stay Hydrated to Thin Mucus
Dehydration leads to thick, sticky mucus that clogs your sinuses and increases pressure. Drinking 8–10 glasses of water daily helps keep mucus thin and promotes natural drainage. Warm fluids like herbal tea, broth, or lemon water are especially effective—they soothe irritated tissues and deliver gentle heat to loosen congestion.
Avoid alcohol and caffeine, which dehydrate and can worsen symptoms. While hydration won’t offer instant relief, it’s one of the most important steps in speeding up recovery.
Expert Note: Warm liquids can also calm inflamed nerves in the jaw, providing mild pain relief.
Breathe in Steam for Immediate Relief
Steam inhalation is one of the fastest ways to open nasal passages and ease sinus pressure. Fill a bowl with hot (not boiling) water, lean over it, and drape a towel over your head to trap the vapor. Breathe deeply for 5–10 minutes, 2–4 times a day.
For added decongestant power, add 2–3 drops of eucalyptus, peppermint, or tea tree oil. These essential oils contain compounds that help break up mucus and reduce inflammation.
Why it works: Moist heat loosens mucus, improves airflow, and reduces pressure on tooth roots.
Apply Warm Compresses to Soothe Facial Pain

Place a warm, damp washcloth over your cheeks, nose, and eye area for 10–15 minutes at a time, up to four times daily. The heat increases blood flow, soothes nerve discomfort, and helps drain congested sinuses.
For enhanced results, try the hot-and-cold compress method:
1. Apply a warm compress for 3 minutes
2. Switch to a cold compress for 30 seconds
3. Repeat the cycle three times
4. Do this up to three times per day
This alternating technique stimulates circulation and reduces swelling faster than heat alone.
Clear Nasal Passages with Saline Irrigation
Use a Neti Pot Safely and Effectively

Saline nasal irrigation flushes out mucus, allergens, and bacteria, directly reducing sinus pressure. Use a neti pot, squeeze bottle, or bulb syringe with a solution of:
– 1/4 to 1/2 tsp non-iodized salt
– 8 oz distilled or previously boiled (then cooled) water
Tilt your head over a sink, pour the solution into one nostril, and let it drain out the other. Repeat on the opposite side. Perform once or twice daily during active symptoms.
Critical Safety Tip: Never use tap water. It can carry harmful organisms like Naegleria fowleri, which can cause rare but fatal infections.
Pro Tip: Perform irrigation before bedtime to reduce overnight congestion and morning pain.
Run a Humidifier at Night
Dry air irritates nasal tissues and thickens mucus, worsening sinus pressure. A cool- or warm-mist humidifier in your bedroom keeps the air moist and supports natural drainage.
Aim to maintain 40–60% indoor humidity. Clean the humidifier regularly to prevent mold and bacteria buildup.
Best for: Allergy sufferers and those in dry climates or heated indoor environments.
Use OTC Medications Strategically
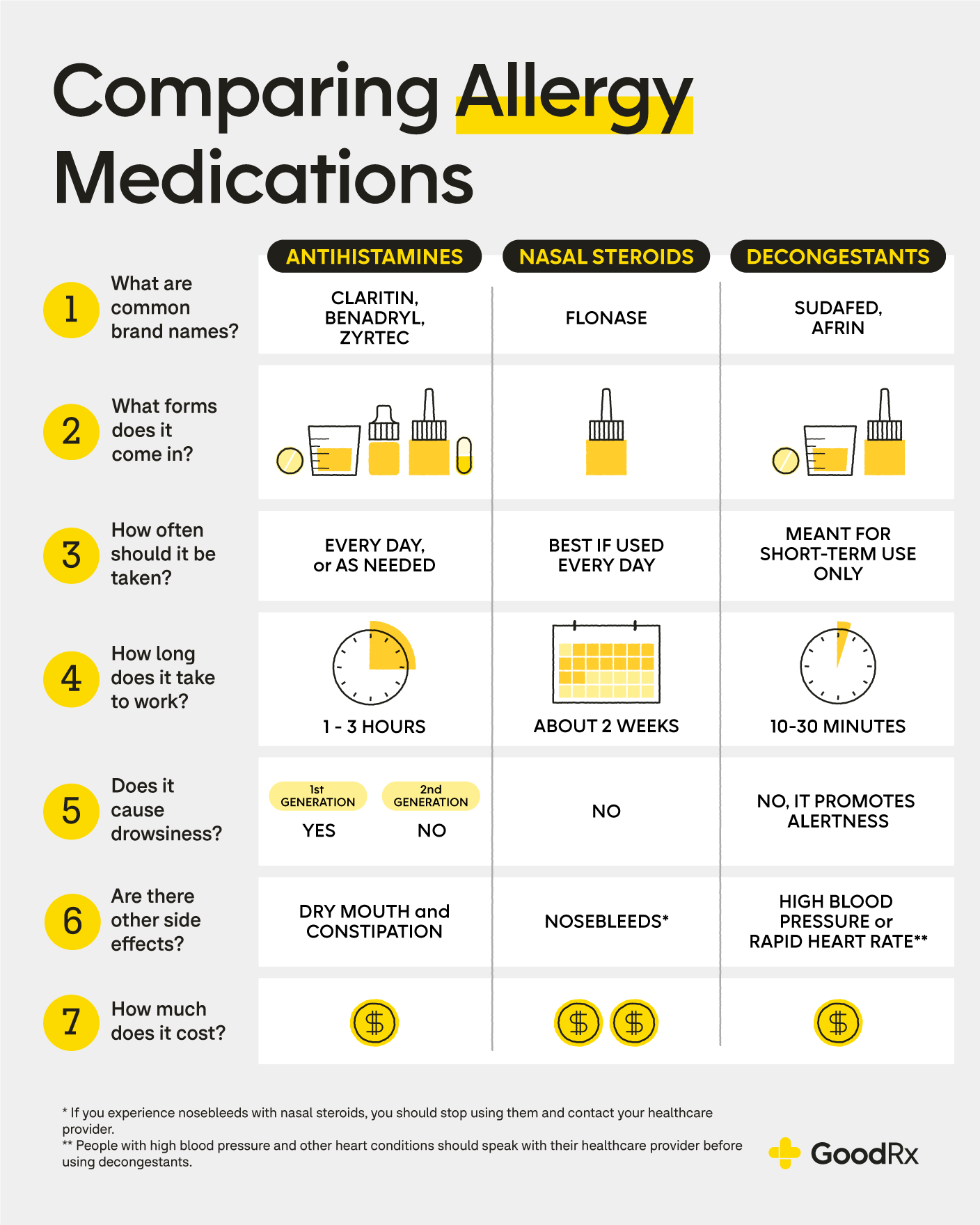
Choose the Right Pain Reliever
For immediate pain relief, ibuprofen (Advil, Motrin) is ideal—it reduces both pain and inflammation. Take it with food to protect your stomach. If NSAIDs aren’t suitable, acetaminophen (Tylenol) relieves pain but doesn’t reduce swelling.
Avoid aspirin in children and teens due to the risk of Reye’s syndrome.
When to take it: At the first sign of pain for best results.
Decongestants to Reduce Nasal Swelling
Oral decongestants like pseudoephedrine (Sudafed) reduce nasal swelling and improve airflow. Nasal sprays such as oxymetazoline (Afrin) work faster but should not be used for more than 3 consecutive days—prolonged use can cause rebound congestion (rhinitis medicamentosa).
Use sprays only as a short-term solution.
Caution: Decongestants can raise blood pressure. Avoid if you have heart conditions or hypertension.
Add Antihistamines for Allergy-Related Congestion
If allergies are behind your sinus pressure, loratadine (Claritin), cetirizine (Zyrtec), or fexofenadine (Allegra) can help. These non-drowsy antihistamines block allergic reactions that lead to congestion.
Avoid older antihistamines like diphenhydramine (Benadryl) at night unless sleep aid is needed—they can thicken mucus and slow drainage.
Pair with hydration: Antihistamines dry mucus membranes, so drink extra water.
Support Healing with Lifestyle Habits
Elevate Your Head While Sleeping
Lying flat allows mucus to pool in the sinuses, increasing pressure overnight. Prop up your head with extra pillows so it’s above heart level. This uses gravity to promote drainage and reduce morning facial pain.
Simple fix: Use a wedge pillow for comfort and consistent positioning.
Try Spicy Foods and Humming
Spicy foods containing capsaicin—like chili peppers, horseradish, or wasabi—can stimulate mucus flow and open nasal passages. While not a cure, they may offer temporary relief.
Surprisingly, humming also helps. A 2006 study found that humming increases nitric oxide in nasal passages, improving airflow and sinus ventilation.
Try it: Hum your favorite tune for 1–2 minutes, 2–3 times a day.
Eat Anti-Inflammatory Foods
Support healing with a diet rich in:
– Ginger and turmeric – natural anti-inflammatories
– Leafy greens and berries – high in antioxidants
– Omega-3 fatty acids – found in salmon, flaxseeds, and walnuts
These foods help reduce overall inflammation, potentially shortening the duration of sinus symptoms.
Maintain Oral Hygiene to Avoid Confusion
Even though the pain isn’t dental, don’t skip your routine. Brush gently with a soft-bristled toothbrush and floss daily to rule out secondary issues.
Use warm saltwater rinses (1/2 tsp salt in 8 oz warm water) 2–3 times daily to soothe oral tissues and reduce inflammation. Avoid very hot or cold drinks that might irritate sensitive nerves.
Why it matters: Good oral hygiene prevents misdiagnosis and protects against infections that could complicate sinus health.
Know When to See a Doctor
Watch for Red Flag Symptoms
Most sinus toothaches resolve within a week or two. But seek medical care if you have:
– Pain lasting more than 7–10 days
– Thick yellow or green nasal discharge
– Fever above 100.4°F (38°C)
– Severe facial swelling or redness
– Vision changes or eye pain
– Stiff neck, confusion, or severe headache
These signs may indicate bacterial sinusitis or a more serious complication, such as orbital or intracranial spread.
Urgent care needed: High fever with facial swelling requires immediate evaluation.
Get Prescription Treatments When Needed
Antibiotics for Bacterial Sinus Infections
If symptoms persist beyond 10 days or worsen after initial improvement, your doctor may prescribe amoxicillin or doxycycline for bacterial sinusitis. Antibiotics are not effective for viral infections, which cause most cases.
Only take antibiotics when prescribed. Overuse contributes to resistance.
Nasal Corticosteroid Sprays for Chronic Inflammation
Fluticasone (Flonase) or mometasone (Nasonex) reduce sinus inflammation, especially in allergy-related or chronic cases. Use daily as directed—effects build over several days.
Best for: Recurrent sinus pressure due to allergies.
Oral Steroids for Severe Cases
Short-term prednisone may be prescribed for acute, severe inflammation. It’s powerful but reserved for significant swelling due to potential side effects.
Not a long-term solution: Used only under medical supervision.
Prevent Future Episodes
Manage Allergies Proactively
Allergic rhinitis is a major trigger. Use saline sprays, antihistamines, and nasal steroids during allergy season. Consider seeing an allergist for testing and immunotherapy if symptoms are frequent.
Install HEPA filters at home and wash bedding weekly to reduce exposure to pollen, dust mites, and mold.
Stay Hydrated Year-Round
Make hydration a habit, not just during illness. Carry a water bottle and sip throughout the day. Well-lubricated sinuses are less likely to become inflamed.
Schedule Regular Dental Checkups
Visit your dentist every 6 months for cleanings and exams. This ensures any true dental issues are caught early and prevents odontogenic sinusitis—a rare condition where a tooth infection spreads to the sinus.
Did you know? Poor dental health can cause sinus problems, not just mimic them.
Summary: Fast Relief Action Plan
- Hydrate – Drink water, broth, or herbal tea
- Steam – Inhale warm vapor 2–4 times daily
- Compress – Apply warm (or alternating hot/cold) cloths to face
- Irrigate – Use saline rinse with sterile water
- Medicate – Take ibuprofen and decongestants as needed
- Elevate – Sleep with head raised
- Humidify – Run a humidifier at night
If pain lasts more than 10 days or you develop fever or swelling, see a doctor. If dental symptoms appear, see a dentist.
Final Note: Tooth pain from sinus pressure is uncomfortable but manageable. By treating the sinuses—not the teeth—you can find fast, effective relief. The key is accurate diagnosis: when in doubt, get checked by both a dentist and physician to ensure no serious condition is missed. With the right approach, most cases resolve fully within two weeks.