Throbbing jaw pain, a pimple-like bump on your gum, or sudden swelling in your cheek could mean you have an abscessed tooth—a dangerous pocket of pus caused by a bacterial infection. Left untreated, this condition doesn’t just destroy your tooth and jawbone—it can spread to your neck, brain, or bloodstream, leading to life-threatening complications like sepsis or Ludwig’s angina. While home remedies may dull the pain temporarily, only professional dental treatment can eliminate the infection for good.
This guide breaks down exactly how to treat an abscessed tooth, from emergency pain relief to long-term solutions. You’ll learn the warning signs, when to go to the ER, what treatments actually work, and how to prevent future infections—all based on clinical evidence and expert dental protocols.
Recognize the Warning Signs
Acting fast starts with knowing what to look for. The earlier you identify an abscess, the better your chances of saving the tooth and avoiding serious complications.
Key Symptoms of a Tooth Abscess
- Persistent, throbbing tooth pain that radiates to your jaw, ear, or neck
- Sensitivity to hot, cold, or chewing pressure
- Swelling in the face, cheek, or jaw
- Fever, chills, or night sweats
- Pus draining from a gum boil (looks like a pimple near the tooth)
- Foul taste in the mouth or chronic bad breath (halitosis)
- Swollen, tender lymph nodes under the jaw or neck
⚠️ Critical insight: If the pain suddenly stops, it doesn’t mean healing—it likely means the nerve inside the tooth has died. The infection is still active and spreading through bone and tissue.
Immediate Home Relief (Temporary Only)
While you must see a dentist, these steps can help manage symptoms until your appointment.
Use Warm Saltwater Rinses
Mix ½ teaspoon of salt in ½ cup of warm water. Swish gently for 30 seconds, then spit. Repeat 3 times daily, especially after meals.
- Why it works: Reduces gum inflammation, flushes out debris, and may encourage minor drainage.
- Best for: Early discomfort or after professional drainage.
Apply a Cold Compress
Wrap ice in a clean cloth and apply it to the outside of your cheek for 10–20 minutes at a time, with 20-minute breaks in between.
- Targets: Swelling, facial puffiness, and nerve-related pain.
- Never use heat—it increases blood flow and can worsen the infection.
Take Over-the-Counter Painkillers
- Ibuprofen (200–400 mg) every 6 hours: Best choice because it fights both pain and inflammation.
- Acetaminophen (500–1000 mg) every 6 hours: Use if you can’t take NSAIDs.
- Avoid aspirin—never place it directly on the gum (it can burn tissue), and its blood-thinning effect raises bleeding risk.
✅ Pro tip: Alternate ibuprofen and acetaminophen every 3 hours (e.g., ibuprofen at 9 AM, Tylenol at 10:30 AM) for stronger relief—just follow dosage guidelines.
Try Clove Oil for Numbing
Dilute 3–5 drops of clove oil in 1 tablespoon of coconut or olive oil. Soak a cotton ball and apply to the affected area for 2–3 minutes, up to 3 times daily.
- Active ingredient: Eugenol, a natural antiseptic and local anesthetic.
- Caution: Never use undiluted—can irritate or damage gum tissue.
Other Natural Aids (Complementary Use Only)
- Hydrogen peroxide rinse (1:2 ratio with water): Swish and spit—kills bacteria and reduces plaque.
- Baking soda rinse (½ tsp baking soda + ½ cup water + pinch of salt): Neutralizes acid and soothes gums.
- Garlic paste: Crush a fresh clove and apply briefly; allicin has antimicrobial properties.
- Oil pulling (swish 1 tbsp coconut oil for 15–20 min): May reduce bacterial load, though clinical evidence is limited.
❌ Myth alert: These remedies do not kill the infection. They only offer temporary symptom relief.
When to Go to the ER Now

Some signs mean the infection is spreading beyond your mouth—and fast.
Emergency Symptoms
- Severe facial or neck swelling
- Difficulty breathing, swallowing, or opening your mouth
- High fever (over 101°F / 38.3°C)
- Red streaks spreading from the jaw
- Confusion, dizziness, or rapid heartbeat
⚠️ These may signal Ludwig’s angina, sepsis, or mediastinitis—conditions with mortality rates as high as 40%. Go to the ER immediately.
You may need IV antibiotics, surgical drainage, or airway support. Do not wait.
Professional Dental Treatments That Work
Only a dentist can eliminate the infection and stop the damage.
Drain the Abscess First
Incision and drainage is often the first step.
- The dentist numbs the area and makes a small cut in the gum to release pus.
- A tiny rubber drain may be placed to keep the wound open for continued drainage.
- Provides immediate pressure relief—pain drops within hours.
✅ Outcome: Rapid symptom improvement, but further treatment is still needed.
Save the Tooth: Root Canal Therapy
The gold standard for a periapical abscess (infection at the root tip).
What Happens During a Root Canal?
- Access the pulp chamber through the top of the tooth.
- Remove infected nerve and pulp tissue.
- Clean, shape, and disinfect the root canals.
- Seal the canals with biocompatible material (gutta-percha).
- Place a crown to protect the weakened tooth.
- Sessions: Usually 1–3 visits.
- Success rate: Over 95% with proper aftercare.
- Lifespan: The tooth can last a lifetime if maintained.
✅ Key benefit: You keep your natural tooth—no shifting, no gaps.
Extract If the Tooth Can’t Be Saved
If the tooth is cracked below the gum line, severely decayed, or loose from bone loss, extraction is necessary.
- The dentist removes the tooth and drains the abscess.
- May place antibiotic gel in the socket to prevent dry socket.
- Full healing takes 1–2 weeks.
🔄 Next steps: Consider a dental implant or bridge later to prevent adjacent teeth from drifting.
Apicoectomy: Last Resort for Failed Root Canals
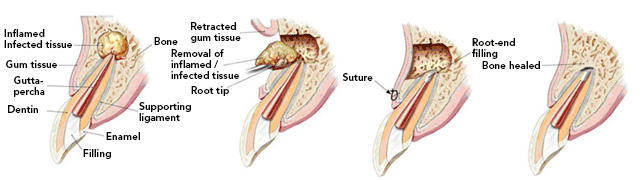
If infection returns after a root canal, an apicoectomy may be needed.
- A surgeon removes the infected tip of the root under local anesthesia.
- Seals the end to prevent reinfection.
- Often completed in one visit.
Do You Need Antibiotics?
Not always—but they’re essential when the infection spreads.
When Antibiotics Are Required
- Facial swelling
- Fever or chills
- Swollen lymph nodes
- Weakened immune system (e.g., diabetes, HIV)
- Signs of systemic infection
Common Prescriptions
| Antibiotic | Dose | For Whom |
|---|---|---|
| Amoxicillin | 500 mg every 8 hours | First-line for most patients |
| Augmentin | 500–875 mg every 12 hours | Severe cases or resistant bacteria |
| Clindamycin | 300–600 mg every 6–8 hours | Penicillin allergy |
| Metronidazole | 500 mg every 8 hours | Combined with penicillin for anaerobes |
❗ Critical rule: Antibiotics alone don’t cure abscesses. Without drainage or dental treatment, the infection will return.
💡 Avoid overuse: Rising resistance due to β-lactamase-producing bacteria makes some antibiotics less effective.
Pain Management After Treatment
Post-procedure discomfort is normal but manageable.
After Drainage or Extraction
- Ibuprofen 400 mg + acetaminophen 500 mg every 6 hours (as directed)
- Cold compress for first 24 hours
- Soft diet: Yogurt, soup, mashed potatoes
- Avoid smoking and alcohol—delays healing
After Root Canal
- Mild soreness for 2–3 days
- Use OTC painkillers as needed
- Avoid chewing on the treated side until the crown is placed
Healing Timeline and Recovery
What to Expect
| Timeframe | What Happens |
|---|---|
| First 24–48 hours | Pain and swelling drop significantly |
| 3–7 days | Infection clears with antibiotics and care |
| 1–2 weeks | Full recovery; extraction site heals |
| Long-term | Root canal-treated tooth functions normally for decades |
✅ Success marker: No pain, no swelling, normal bite, and no gum boil.
Can a Tooth Abscess Heal on Its Own?
No. Even if the pain stops, the infection persists.
- A dead nerve means no more pain signals, not healing.
- Pus continues to destroy jawbone and tissue.
- Risk of sepsis, brain abscess, or mediastinitis (chest infection with 40% mortality).
❌ Never wait it out. Early treatment = simpler, cheaper, safer.
Prevent Future Abscesses
Stop decay and trauma before they lead to infection.
Daily Prevention Habits
- Brush twice daily with fluoride toothpaste
- Floss every night—plaque hides between teeth
- Use antiseptic mouthwash (e.g., chlorhexidine or essential oil-based)
- Limit sugar and starch—they feed cavity-causing bacteria
- Quit smoking—doubles your abscess risk
Regular Dental Care
- See your dentist every 6 months for cleanings and X-rays
- Fix cavities early—before they reach the nerve
- Wear a mouthguard if you grind teeth or play sports
- Treat gum disease—periodontitis leads to periodontal abscesses
Frequently Asked Questions
Can I pop a gum abscess at home?
No. Popping it yourself risks spreading infection, causing cellulitis, or damaging tissue. Let a dentist drain it safely.
What if the abscess bursts on its own?
- Rinse with warm salt water
- Call your dentist immediately
- You still need treatment to remove the infection source
Are natural remedies effective?
Some, like clove oil or saltwater, help with symptoms. But none eliminate the infection. Use only as temporary aids.
How fast can an abscess spread?
In days to weeks, depending on immune health. A small infection can become Ludwig’s angina (neck swelling that blocks airways) rapidly.
Will antibiotics clear the abscess?
They control systemic spread but don’t cure it. You still need drainage or root canal.
Final Takeaways
An abscessed tooth is not just a toothache—it’s a dangerous infection that demands action.
- Home care helps temporarily but won’t cure the problem.
- See a dentist ASAP—the sooner, the better the outcome.
- Root canal or extraction are the only real cures.
- Antibiotics support treatment but aren’t standalone solutions.
- Prevention is simple: Brush, floss, limit sugar, and visit your dentist regularly.
🚨 If you have swelling, fever, or trouble breathing—go to the ER now. Delaying could cost you your life.
Don’t ignore the signs. Call your dentist today—your health depends on it.